Tuberculosis
Overview
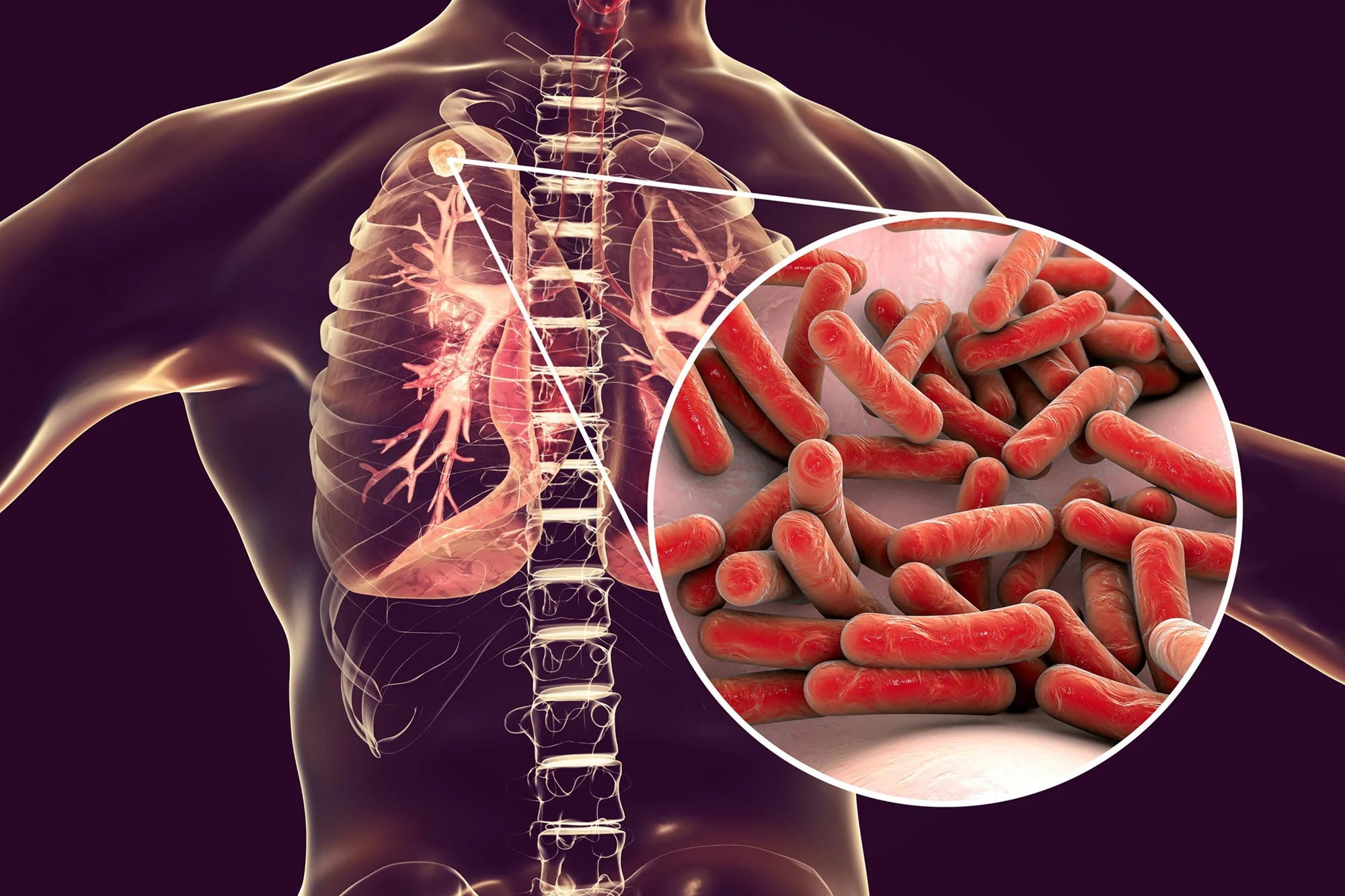
Tuberculosis (TB) is an infectious disease caused by bacteria that most often affects the lungs. It spreads through the air when people with TB cough, sneeze or spit.
Tuberculosis is preventable and curable.
About a quarter of the global population is estimated to have been infected with TB bacteria. About 5–10% of people infected with TB will eventually get symptoms and develop TB disease.
Those who are infected but free of disease cannot transmit it. TB disease is usually treated with antibiotics and can be fatal without treatment.
In certain countries, the Bacille Calmette-Guérin (BCG) vaccine is given to babies or small children to prevent TB. The vaccine prevents deaths from TB and protects children from serious forms of TB.
Certain conditions can increase a person’s risk for TB disease:
- diabetes (high blood sugar)
- weakened immune system (for example, from HIV or AIDS)
- being malnourished
- tobacco use
- harmful use of alcohol.
Key facts
- A total of 1.25 million people died from tuberculosis (TB) in 2023 (including 161 000 people with HIV). Worldwide, TB has probably returned to being the world’s leading cause of death from a single infectious agent, following three years in which it was replaced by coronavirus disease (COVID-19). It was also the leading killer of people with HIV and a major cause of deaths related to antimicrobial resistance.
- In 2023, an estimated 10.8 million people fell ill with TB worldwide, including 6.0 million men, 3.6 million women and 1.3 million children. TB is present in all countries and age groups. TB is curable and preventable.
- Multidrug-resistant TB (MDR-TB) remains a public health crisis and a health security threat. Only about 2 in 5 people with drug resistant TB accessed treatment in 2023.
- Global efforts to combat TB have saved an estimated 79 million lives since the year 2000.
- US$ 22 billion is needed annually for TB prevention, diagnosis, treatment and care to achieve the global target by 2027 agreed at the 2023 UN high level-meeting on TB.
- Ending the TB epidemic by 2030 is among the health targets of the United Nations Sustainable Development Goals (SDGs).
Cause of Tuberculosis
Tuberculosis (TB) is an infectious disease primarily caused by the bacterium Mycobacterium tuberculosis. Transmission occurs when individuals with active pulmonary TB expel infectious aerosol droplets through actions such as coughing, sneezing, speaking, singing, or spitting. These droplets, ranging from 0.5 to 5.0 micrometers in diameter, can remain suspended in the air, facilitating the spread of the disease. A single sneeze can release up to 40,000 droplets, each capable of transmitting the infection.
The World Health Organization (WHO) reports that approximately a quarter of the global population has been infected with TB bacteria. However, only about 5–10% of these individuals will develop active TB disease.
While TB most commonly affects the lungs, it can also impact other parts of the body, including the kidneys, spine, and brain. The disease is preventable and curable, with early detection and appropriate treatment being crucial for effective management.
Diagnosis of Tuberculosis
WHO recommends the use of rapid molecular diagnostic tests as the initial diagnostic test in all persons with signs and symptoms of TB.
Rapid diagnostic tests recommended by WHO include the Xpert MTB/RIF Ultra and Truenat assays. These tests have high diagnostic accuracy and will lead to major improvements in the early detection of TB and drug-resistant TB.
A tuberculin skin test (TST), interferon gamma release assay (IGRA) or newer antigen-based skin tests (TBST) can be used to identity people with infection.
Diagnosing multidrug-resistant and other resistant forms of TB (see multidrug-resistant TB section below) as well as HIV-associated TB can be complex and expensive.
Tuberculosis is particularly difficult to diagnose in children.
Symptoms of Tuberculosis(TB)
People with TB infection don’t feel sick and aren’t contagious. Only a small proportion of people who get infected with TB will get TB disease and symptoms. Babies and children are at higher risk.
TB disease occurs when bacteria multiply in the body and affect different organs. TB symptoms may be mild for many months, so it is easy to spread TB to others without knowing it. Some people with TB disease do not have any symptoms.
Common symptoms of TB are:
- prolonged cough (sometimes with blood)
- chest pain
- weakness
- fatigue
- weight loss
- fever
- night sweats
The symptoms people get depend on which part of the body is affected by TB. While TB usually affects the lungs, it can also involve the kidneys, brain, spine and skin.
Treatment of Tuberculosis
Tuberculosis disease is treated with special antibiotics. Treatment is recommended for both TB infection and disease.
The most common antibiotics used are:
- isoniazid
- rifampicin
- pyrazinamide
- ethambutol.
To be effective, medications need to be taken daily for 4–6 months. It is dangerous to stop the medications early or without medical advice as it can prompt TB bacteria in the body to become resistant to the drugs.
TB that doesn’t respond to standard drugs is called drug-resistant TB and requires treatment with different medicines.
Multidrug-resistant TB (MDR-TB)
Drug resistance emerges when TB medicines are used inappropriately, through incorrect prescription by health care providers, poor quality drugs, or patients stopping treatment prematurely.
MDR-TB is a form of TB caused by bacteria that do not respond to isoniazid and rifampicin, the two most effective first-line TB drugs. MDR-TB is treatable and curable by using other drugs, which tend to be more expensive and toxic.
In some cases, extensively drug resistant TB or XDR-TB can develop. TB caused by bacteria that do not respond to the most effective drugs in MDR-TB treatment regimens can leave patients with very limited treatment options.
MDR-TB remains a public health crisis and a health security threat. Only about 2 in 5 people with multidrug resistant TB accessed treatment in 2023.
In accordance with WHO guidelines, detection of MDR-TB requires bacteriological confirmation of TB and testing for drug resistance using rapid molecular tests or culture methods.
In 2022, new WHO guidelines prioritized a short 6-month all-oral regimen known as BPaLM/BPaL as a treatment of choice for eligible patients. Globally in 2023, 5646 people with MDR/RR-TB were reported to have been started treatment on the BPaLM/BPaL regimen, up from 1744 in 2022. The shorter duration, lower pill burden and high efficacy of this novel regimen can help ease the burden on health systems and save precious resources to further expand the diagnostic and treatment coverage for all individuals in need. In the past, MDR-TB treatment used to last for at least 9 months and up to 20 months. WHO recommends expanded access to all-oral regimens
Prevention and control
Follow these steps to help prevent tuberculosis infection and spread:
- Seek medical attention if you have symptoms like prolonged cough, fever and unexplained weight loss as early treatment for TB can help stop the spread of disease and improve your chances of recovery.
- Get tested for TB if you are at increased risk, such as if you have HIV or are in contact with people who have TB in your household or workplace.
- TB preventive treatment (or TPT) prevents infection from becoming disease. If prescribed TPT, complete the full course.
- If you have TB, practice good hygiene when coughing, including avoiding contact with other people and wearing a mask, covering your mouth and nose when coughing or sneezing, and disposing of sputum and used tissues properly.
- Special measures like respirators and ventilation are important to reduce infection in healthcare facilities and other institutions
WHO’s Stance on Tuberculosis
WHO is working closely with countries, partners and civil society in scaling up the TB response. Six core functions are being pursued by WHO to contribute to achieving the targets of the 2023 UN high-level meeting political declaration, Sustainable Development Goals, End TB Strategy and WHO strategic priorities:
- providing global leadership to end TB through strategy development, political and multisectoral engagement, strengthening review and accountability, advocacy, and partnerships, including with civil society;
- shaping the TB research and innovation agenda and stimulating the generation, translation and dissemination of knowledge;
- setting norms and standards on TB prevention and care and promoting and facilitating their implementation;
- developing and promoting ethical and evidence-based policy options for TB prevention and care;
- ensuring the provision of specialized technical support to Member States and partners jointly with WHO regional and country offices, catalysing change, and building sustainable capacity; and
- monitoring and reporting on the status of the TB epidemic and progress in financing and implementation of the response at global, regional and country levels